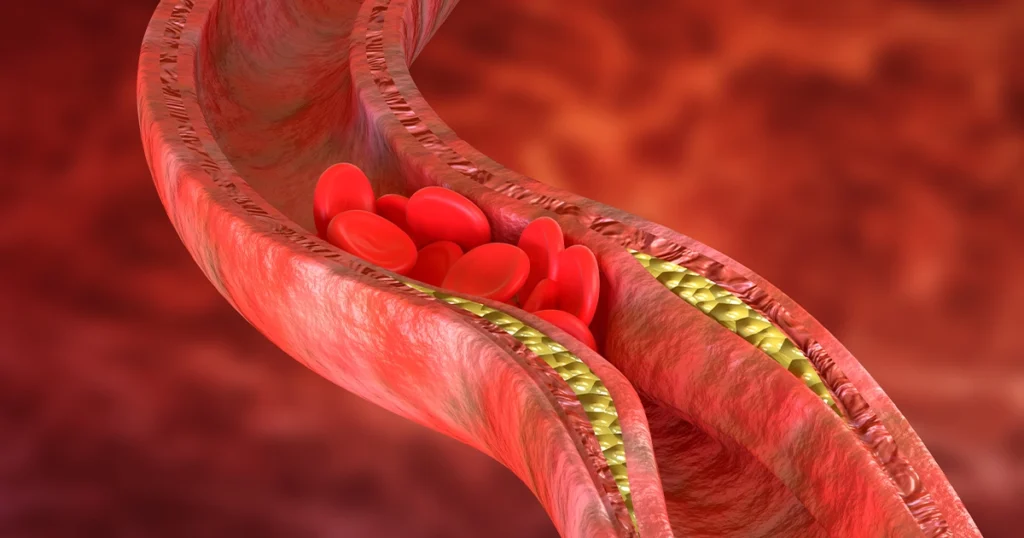
Blood clots are serious medical events that occur when blood thickens and forms a semi-solid mass inside a blood vessel, restricting normal circulation. Understanding What Is A Blood Clot is crucial because timely recognition and care can prevent life-threatening complications such as heart attack, stroke, or pulmonary embolism.
These clots may form during normal healing, like after an injury, but can also develop internally without warning. If you notice concerning symptoms, especially sudden or severe ones, visiting our Laredo emergency room promptly can make a critical difference in your health outcome.
What Does A Blood Clot Look Like
A blood clot usually appears as a gel-like mass of dark red blood, similar in appearance to coagulated jelly. Clots form when platelets and proteins such as fibrin stick together to stop bleeding, but they can also form inappropriately inside veins or arteries.
A systematic review reported that approximately 21% of hospitalized COVID‑19 patients developed thrombotic events, such as deep vein thrombosis or pulmonary embolism, highlighting the high risk of blood clots during severe illness.
Blood Clot Symptoms
- Sudden swelling in a leg or arm.
- Pain or tenderness in a limb.
- Warmth and redness over the affected area.
- Sudden shortness of breath or difficulty breathing.
- Chest pain that worsens with deep breaths.
How Do Blood Clots Form
Blood clots form when platelets and clotting proteins accumulate in response to blood vessel injury, slowing or stopping bleeding. While protective in normal healing, clots can also form abnormally when blood flow slows, the vessel lining is damaged, or the clotting system is overactive. Risk factors include immobility, certain medical conditions, and genetic predispositions.
Where Are Blood Clots Located?
Blood clots can form in many parts of the body and may disrupt blood flow wherever they occur. The location of a clot determines its symptoms, severity, and urgency of treatment. Some clots remain stationary, while others travel through the bloodstream and lodge in vital organs, causing serious complications.
- Leg Veins (Deep Vein Thrombosis): Usually forms in deep veins of the legs or thighs, causing swelling, pain, and warmth.
- Lungs (Pulmonary Embolism): Occurs when a clot travels to the lungs, leading to sudden shortness of breath, chest pain, or rapid heartbeat.
- Heart Arteries: Can block blood flow to the heart, resulting in a heart attack with chest discomfort and sweating.
- Brain Arteries: Clots here may cause a stroke, with sudden weakness, difficulty speaking, or vision problems.
- Abdominal Vessels: Clots in abdominal vessels can cause severe abdominal pain and digestive issues.
What Causes Blood Clots
Blood clots occur when blood flow slows, the vessel wall is damaged, or clotting mechanisms are overactive. Often, multiple factors contribute simultaneously, increasing the risk of abnormal clot formation.
Prolonged Immobility
Extended periods of sitting or lying down, such as during long flights, car trips, or bed rest, can slow blood flow in the veins, allowing platelets and proteins to form a clot. This slowed circulation can also increase the risk of swelling and stiffness in the legs, which may go unnoticed until a clot develops.
Medical Conditions
Certain illnesses, including cancer, heart disease, and infections, disrupt normal clotting and increase clot risk. Inherited clotting disorders also raise susceptibility. Some chronic conditions, like diabetes, can further alter blood composition and make clots more likely.
Surgery or Injury
Major surgery or physical trauma can damage blood vessels and slow blood flow, increasing the likelihood of clot formation, especially without early movement after procedures. Even minor injuries in combination with other risk factors can occasionally trigger clot formation in susceptible individuals.
Hormones and Pregnancy
Hormonal changes from birth control, hormone therapy, or pregnancy increase clotting risk. Pregnant and postpartum women are particularly vulnerable. Hormonal fluctuations can also affect blood vessel flexibility, contributing to altered blood flow and clot risk.
Do Blood Clots Go Away?
Yes, some clots can dissolve on their own or with medical treatment, but many require anticoagulant therapy to help the body break them down safely. Early treatment improves outcomes and helps prevent complications or recurrence.
Do Blood Clots Hurt?
Blood clots may or may not cause pain depending on their size and location. Some people feel significant discomfort, while others notice subtle symptoms. Pain often comes with swelling or warmth in the affected area, but clots in organs like the lungs or brain can produce different types of symptoms.
- Localized pain or tenderness in a limb.
- Warmth and redness over the affected area.
- Sudden shortness of breath.
- Chest discomfort with breathing.
Contact the STAT Specialty Hospital immediately if you experience these symptoms, as rapid assessment and treatment can be life‑saving.
How To Get Rid Of Blood Clots
Treating blood clots involves stopping further clotting, preventing growth of the existing clot, and promoting safe breakdown. Treatment plans are individualized, based on where the clot is, your overall health, and whether you’ve had clots before. Prompt treatment from a medical professional reduces complications and improves recovery.
Anticoagulant Medications
Also called blood thinners, these medications prevent clots from growing and lower the risk of new clots forming. Doctors carefully prescribe these based on your clot location, health status, and bleeding risk, and they monitor blood tests regularly to ensure safe dosing.
Thrombolytic Therapy
In severe cases, clot-dissolving drugs are administered to break up large clots quickly, often in emergency settings. Physicians only recommend this therapy for life-threatening clots and closely monitor patients in a hospital setting to manage potential bleeding complications.
Surgical or Catheter‑Based Removal
For large or dangerous clots, procedures may physically remove the clot and restore blood flow. Doctors decide on these interventions when medications are insufficient or rapid restoration of blood flow is critical, usually in specialized hospital settings.
Lifestyle and Prevention Measures
Maintaining mobility, wearing compression stockings, and addressing risk factors like obesity, smoking, or sedentary behavior help prevent future clots. These measures are typically recommended by healthcare providers as part of a comprehensive treatment plan alongside medications or procedures.
Care For Blood Clots At STAT Specialty Hospital
If you notice signs of a blood clot, prompt evaluation is essential to prevent serious complications. At STAT Specialty Hospital, our experienced team provides rapid assessment, accurate diagnosis, and personalized treatment plans. Understanding What Is A Blood Clot ensures patients receive safe, timely care to protect their health.
Managing blood clots often requires continuous monitoring, which is why our center offers comprehensive inpatient care. Patients receive close observation, supportive interventions, and guidance from specialists to reduce risks. STAT Specialty Hospital is dedicated to helping patients recover safely and prevent further complications.