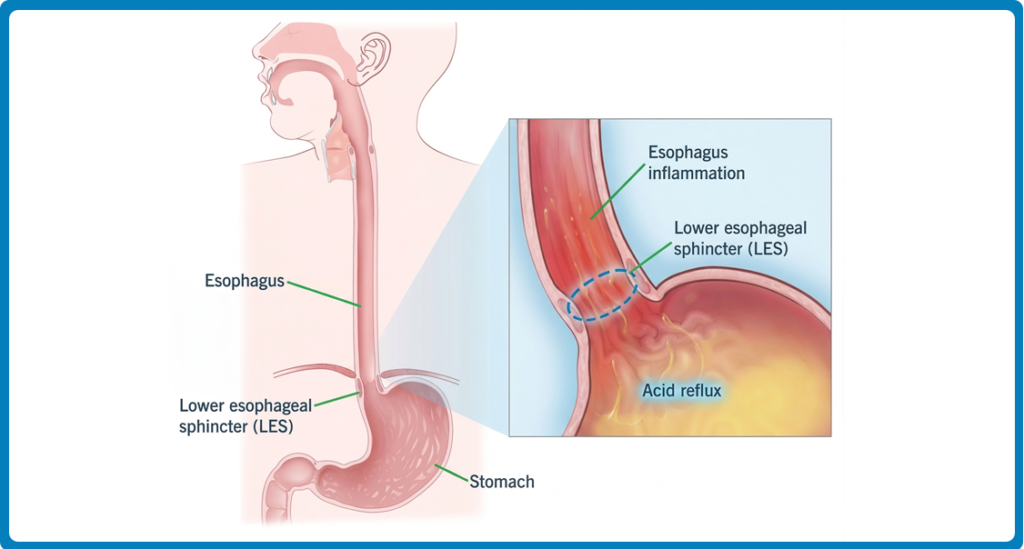
Acid reflux is a digestive disorder that occurs when stomach acid flows backward into the esophagus instead of staying in the stomach. The esophagus is a sensitive tube connecting the throat to the stomach, and unlike the stomach, it lacks a protective lining to withstand acid. When acid enters this area, it can cause irritation, burning, and discomfort. This condition can range from occasional mild reflux to more persistent digestive issues.
The backward flow of acid usually happens when the lower esophageal sphincter (LES), a muscular valve at the base of the esophagus, becomes weak or relaxes at the wrong time. Normally, the LES opens to allow food into the stomach and closes tightly to prevent acid from rising. Occasional reflux often occurs after large meals or certain trigger foods. Frequent episodes may indicate gastroesophageal reflux disease (GERD), a chronic condition that can lead to complications if left untreated. In severe cases with intense chest pain or complications, seeking immediate care at an emergency room Laredo, TX is essential to ensure proper diagnosis and treatment.
Key Takeaways
- Acid reflux occurs when stomach acid enters the esophagus.
- Many people experience occasional symptoms.
- Frequent reflux may indicate GERD.
- Lifestyle changes and medications are effective.
- Require immediate medical attention.
How to Stop Acid Reflux
Managing acid reflux requires a combination of consistent habits and, in some cases, medical treatment. The goal is to reduce acid production, prevent backflow, and protect the esophagus from irritation.
Lifestyle Changes
Lifestyle adjustments are one of the most effective and natural ways to control acid reflux symptoms. These changes focus on improving digestion and reducing pressure on the stomach, which helps prevent acid from moving upward into the esophagus.
Eating smaller meals throughout the day instead of large portions allows the stomach to process food more efficiently. Large meals tend to stretch the stomach and increase pressure, making reflux more likely. Additionally, avoiding lying down immediately after eating is important because gravity plays a key role in keeping stomach acid in place.
Maintaining a healthy body weight also significantly reduces the risk of acid reflux. Excess weight around the abdomen puts pressure on the stomach, pushing acid toward the esophagus. Even a small amount of weight loss can lead to noticeable improvement in symptoms.
- Eat Smaller Meals: Helps prevent excessive stomach pressure and improves digestion.
- Avoid Trigger Foods: Reduces irritation and lowers the chance of reflux episodes.
- Stay Upright After Eating: Allows gravity to keep acid in the stomach.
- Maintain Healthy Weight: Minimizes pressure on the digestive system.
Over-the-Counter Medications
Over-the-counter medications are widely used to manage acid reflux, especially for individuals who experience occasional symptoms. These medications work in different ways, either by neutralizing stomach acid or reducing its production.
Antacids are often the first choice because they provide quick relief. They work by neutralizing existing acid in the stomach, which can help relieve symptoms like heartburn almost immediately. However, their effects are usually short-lived.
H2 blockers and proton pump inhibitors (PPIs) are more effective for longer-lasting relief. H2 blockers reduce the amount of acid produced by the stomach, while PPIs block acid production more significantly and are often recommended for frequent symptoms.
- Antacids: Provide fast relief by neutralizing stomach acid.
- H2 Blockers: Reduce acid production for extended symptom control.
- PPIs: Offer a strong and long-lasting reduction in acid levels.
Prescription Treatments
For individuals with persistent or severe acid reflux, prescription treatments may be necessary. These treatments are typically recommended when lifestyle changes and over-the-counter medications do not provide sufficient relief.
Doctors may prescribe stronger versions of H2 blockers or PPIs to better control acid production. In addition, diagnostic tests such as endoscopy may be used to examine the esophagus and identify any damage caused by prolonged acid exposure.
In some cases, long-term management plans are developed to prevent complications such as inflammation or narrowing of the esophagus. Early medical intervention can help reduce the risk of serious digestive issues, and in urgent situations, visiting an emergency room near me can provide immediate care and evaluation.
- Stronger Medications: Provide more effective acid control.
- Medical Evaluation: Identifies underlying causes and complications
What Causes an Acid Reflux?
Acid reflux can develop due to several factors that either weaken the LES or increase pressure within the stomach. Understanding these causes is essential for prevention and long-term management.
- Weak Lower Esophageal Sphincter: The LES fails to close properly, allowing acid to escape.
- Dietary Triggers: Foods like spicy meals, chocolate, caffeine, and citrus can worsen symptoms.
- Overeating: Large meals increase stomach pressure and promote reflux.
- Obesity: Extra abdominal weight pushes stomach contents upward.
- Pregnancy: Hormonal changes and physical pressure increase reflux risk.
What Happens During Acid Reflux
Acid reflux is not just a simple discomfort, it involves a series of physiological changes in the digestive system that can lead to irritation and long-term damage if repeated frequently.
When the LES does not function properly, stomach acid travels upward into the esophagus. This acid is strong enough to break down food, so when it comes into contact with the delicate lining of the esophagus, it causes a burning sensation and inflammation.
Over time, repeated exposure to acid can damage the esophageal lining, leading to complications such as ulcers or narrowing of the esophagus. This is why managing acid reflux early is important for maintaining digestive health.
- LES Dysfunction: The valve fails to prevent acid movement.
- Acid Irritation: The esophagus becomes inflamed.
- Chronic Exposure: Leads to long-term damage if untreated.
Symptoms of Acid Reflux
The symptoms of acid reflux can vary from mild to severe and may affect daily comfort and quality of life.
- Heartburn: A burning sensation in the chest, often after eating or at night.
- Sour Taste in Mouth: Caused by acid reaching the throat.
- Regurgitation: Food or liquid coming back into the throat.
- Nausea: Feeling sick or uncomfortable after meals.
- Difficulty Swallowing: A sensation of food being stuck.
- Chronic Cough: Persistent throat irritation.
How Long can Acid Reflux Last?
The duration of acid reflux symptoms depends on the underlying cause and individual lifestyle factors.
- Mild Episodes: Usually last a few minutes and resolve naturally.
- After Large Meals: Symptoms may persist for several hours.
- Nighttime Reflux: Can last longer due to lying down.
- Chronic GERD: May require ongoing treatment.
Acid Reflux vs Heartburn vs GERD
These terms are often confused but represent different aspects of the same condition.
- Acid Reflux: The actual movement of acid into the esophagus.
- Heartburn: The burning sensation caused by acid irritation.
- GERD: A chronic condition involving frequent reflux episodes.
When to Go to the Emergency Room for Acid Reflux
While most cases are manageable, certain symptoms require immediate medical attention.
- Severe Chest Pain: Especially if it spreads to other areas.
- Difficulty Breathing: May indicate a serious issue.
- Persistent Vomiting: Requires urgent care.
- Swallowing Problems: Could signal complications.
If you experience any of these symptoms, it is important to seek immediate medical attention. Visiting STAT Specialty Hospital can provide prompt evaluation, accurate diagnosis, and the necessary treatment to prevent serious complications.
Care for Acid Reflux Concerns at STAT Specialty Hospital
Patients at STAT Specialty Hospital receive comprehensive evaluation and treatment for acid reflux and GERD. Physicians assess the lower esophageal sphincter function and examine symptoms including heartburn, throat irritation, and bloating. Diagnostic procedures, such as esophageal manometry and endoscopy, allow for precise identification of reflux severity and tissue damage. Treatment plans often combine over-the-counter or prescription medications with lifestyle adjustments and dietary counseling. Continuous follow-up ensures symptom control and prevents chronic complications. Urgent care is available for severe symptoms like chest pain, breathing difficulties, or vomiting. The hospital focuses on improving patient comfort, reducing flare-ups, and promoting long-term digestive wellness. For younger patients experiencing severe reflux symptoms, specialized Pediatric emergency services are available to provide prompt, child-focused care and ensure safe, effective treatment.
FAQs
Is acid reflux dangerous?
Mild reflux is generally manageable, but chronic reflux (GERD) can damage the esophagus. Long-term complications include ulcers, strictures, or Barrett’s esophagus. Timely lifestyle changes and treatment reduce potential risks.
Can acid reflux cause nausea?
Yes, acid reflux can irritate the stomach and esophagus, leading to nausea or an unsettled stomach. Symptoms often worsen after heavy or spicy meals. Persistent nausea should be evaluated by a healthcare provider.
Is yogurt good for acid reflux?
Plain, low-fat yogurt can help soothe the stomach and improve digestion due to probiotics. Avoid flavored or full-fat varieties, as sugar and fat can worsen reflux. Eating small portions is generally recommended.

